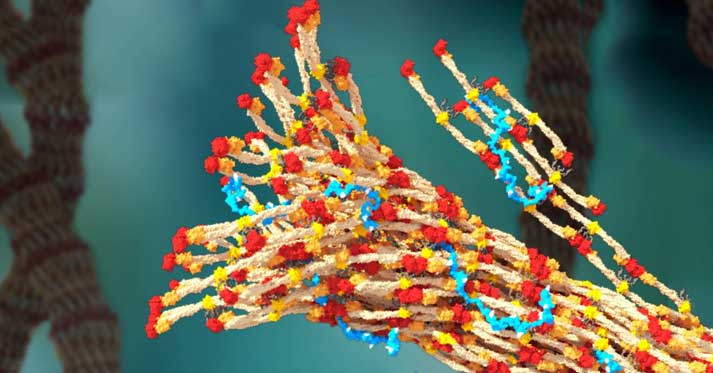
A research team at the University of Washington has developed a synthetic polymer that mimics natural clotting factors to quickly control severe bleeding. In rodent studies, the injectable polymer — known as PolySTAT — reduced blood loss and dramatically improved survival rates. If shown to be effective in humans, it could help improve survival for trauma victims in remote, rural and battlefield settings.
The PolySTAT development team described their initial studies in a paper published March 4 in Science Translational Medicine. According to the paper, about one-quarter of trauma patients develop trauma-induced coagulopathy:
- Large-volume blood loss rapidly depletes clotting factors, preventing the formation of strong fibrin networks within blood clots.
- Severe bleeding also triggers hyperfibrinolysis, or the accelerated breakdown of fibrin matrices.
- The weak blood clots that result are unable to withstand the pressure of circulating blood.
- The blood clots break away, leading to continued bleeding.
To solve the problem of trauma-induced coagulopathy, the research team looked to Factor XIIIa, according to the paper. This natural enzyme stabilizes blood clots by creating cross-links within fibrin networks. “Drawing inspiration from FXIIIa, we engineered a synthetic hemostatic polymer, PolySTAT, that stabilizes blood clots through fibrin cross-linking.”
Stronger clots, better survival
PolySTAT is delivered by injection. It circulates innocuously in the blood until it activates at the site of a vascular injury.
During initial tests, rats were randomized into five treatment groups of five rats each. After receiving a femoral artery injury, researchers administered PolySTAT, PolySCRAM, hFXIIIa, rat albumin or saline. All five rats treated with PolySTAT survived. Survival in other treatment groups ranged from zero to 40%.
The researchers found that PolySTAT reduced blood loss and improved tissue perfusion while reducing fluid resuscitation requirements. “When evaluated in vitro under coagulopathic and hyperfibrinolytic
conditions, PolySTAT accelerated clotting kinetics, increased clot strength, and delayed clot breakdown.”
Minimal risks
PolySTAT appears to minimize the risk of stroke or heart attack. The polymer binds to fibrin, not circulating fibrin precursor. This localizes its activity at the site of the injury and minimizes the risk of thrombosis.
After stabilization, the cross-linked clots can be removed surgically or allowed to dissolve through natural clot breakdown.
“PolySTAT-modified clots will break down naturally, just taking a little longer to do so,” said Leslie W. Chan, lead author of the study. “The polymer was designed to have this effect so that the clot would have longer residence time at the injury site to account for transport time to a hospital, where surgical intervention is then used to repair the injury. We are also currently working on reversible systems.”
Field use
The PolySTAT development team includes Nathan White, MD, MS, an assistant professor of emergency medicine who treats patients at Harborview Medical Center, a Level I trauma center.
Dr. White said synthetic polymers offer several advantages over natural blood products, according to a UW news release. Polymers reduce infection and transfusion risks, and they are well suited to field use, especially in remote settings. “This is something you could potentially put in a syringe inside a backpack and give right away to reduce blood loss and keep people alive long enough to make it to medical care,” he said.