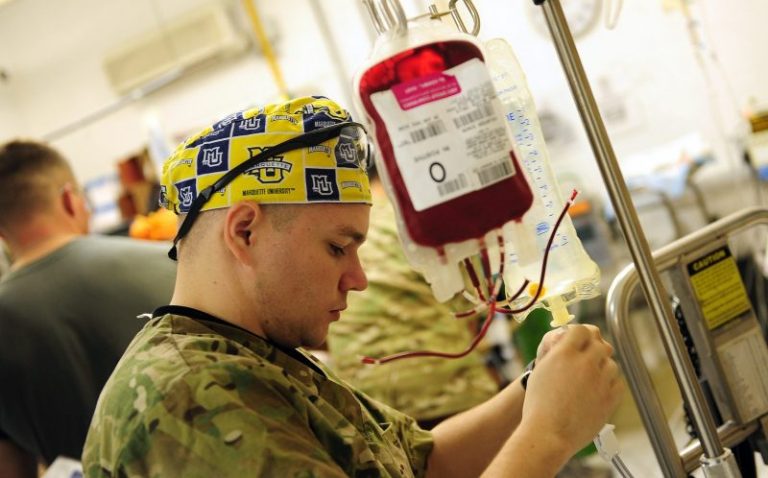
Before they ever laid eyes on the twenty-four-year-old soldier, the Forward Surgical Team in remote Afghanistan was notified of his critical condition and started to prepare.[3] The young man had been strafed with an AK-47, an assault rifle designed to kill with stunning efficiency. Multiple rounds struck his torso and legs, each two-inch bullet traveling at 2,350 feet per second, capable of piercing the metal of a car door and killing its intended target inside.
His surgeons were well acquainted with how bullets like these tear through the human body, leaving a meandering trail of destruction like a tornado through a trailer park. They also knew that if they could control massive hemorrhage, the most common cause of preventable death in combat casualties, they might be able to save a life. From the reports they were getting en route, the soldier was already sinking into shock, a lack of adequate circulation in the body from a massive loss of blood. His only chance at survival would be a flawless execution of the medical team’s resuscitation game plan.
UP TO 16 PERCENT of patients who die from hemorrhage might have been saved if bleeding had been recognized earlier and treated effectively.[4] Undetected internal bleeding into the abdomen or pelvis usually accounts for most of these preventable deaths. But a trauma victim can also bleed to death from external hemorrhage, like bleeding from an arm or leg that no one manages to control in time. Applying a tourniquet, a ten-second procedure, might have saved him.
Armed with statistics such as these, trauma surgeons are starting to reshuffle the deck on priorities in resuscitation, particularly in combat. For the better part of a half-century, the “controlling bleeding” part has been the third priority in Advanced Trauma Life Support classes, behind airway and breathing problems, because these were considered the most immediate threats to life.
“Stop bleeding,” however, is climbing the priority list thanks largely to the efforts of military physicians who discovered that most combat casualties die within ten minutes of being wounded, and usually from exsanguination.[5] In a one-year period, ten soldiers were dead on arrival to a Baghdad combat support hospital after isolated limb exsanguinations.[6]
The military’s MARCH protocol (Massive Hemorrhage, Airway, Respirations, Circulation, and Hypothermia) now instructs army medics to stop external bleeding before doing anything else.[7] Direct pressure is applied first. If the bleeding continues and the source is an extremity, a tourniquet is applied above the site of bleeding.
Tourniquets fell out of favor and were shelved during World War II and Vietnam due to the concern over impairing the blood supply to a limb and damaging it further. But they have made a comeback based on a decade of combat experience in Iraq and Afghanistan.[8] The combat application tourniquet is a simple tourniquet that can be applied by a wounded soldier with the use of only one hand.[9] Applying a tourniquet before a patient goes into shock can improve survival by 90 percent. Because of the favorable results from using tourniquets, the morbidity of extreme blood loss, and the ease of use, they are becoming part of standard civilian EMS procedure once again, and some are suggesting that other first responders, such as police, carry them too.
Hemostatic bandages, like QuikClot Combat Gauze, are bandages impregnated with kaolin, an agent that accelerates the body’s ability to form a blood clot and therefore stop active bleeding in a wound.[10] These bandages can stem bleeding in anatomic areas that cannot be easily compressed or controlled with a tourniquet, such as the axilla or groin.
Tracking down the source of internal bleeding will usually require a more in-depth investigation utilizing imaging studies such as a CAT scan or bedside ultrasound to try and pinpoint the body cavity and organ source. Even if the exact location isn’t known, innovative solutions are emerging to compress internal bleeding until a wounded victim can make it to the hospital.
In the “medical version of Fix-a-Flat,” a syringe full of small spongelike discs impregnated with a clotting agent can be injected into an open wound like a bullet hole in the abdomen.[11] The sponges expand to ten times their size within seconds to plug the wound and internally compress bleeding sites. This device, the XStat, is exactly the type of tool that could stabilize a soldier on the battlefield until he can reach a hospital. Approved by the Food and Drug Administration (FDA) in 2014, the XStat is now available in both the military and civilian markets.

BY THE TIME the young soldier arrived at the field hospital, his heart was in overdrive at 150 beats per minutes, his blood pressure dipping below 70 mm Hg, and his abdomen felt swollen and tight from the blood accumulating inside. Medics hung blood and plasma and rolled him into an operating room where surgeons stood scrubbed and gowned.
Simply inducing anesthesia, which causes dilation of the blood vessels, could be enough to collapse his cardiovascular system, so instead of the usual sequence of putting the patient under and then prepping and draping, the doctors reversed the order, prepping first, and then stood by. This way, if the patient crashed they could quickly open his abdomen.
As soon as the anesthetic drugs were given, the patient’s blood pressure dipped further, prompting the surgeons to immediately open his abdomen through a midline incision. As they pressed the knife into the layers of the abdominal wall and through the peritoneal lining of the abdominal cavity, blood spurted out of the incision and across the drapes. The well-rehearsed team responded automatically to the profuse rush of blood, packing each quadrant of the abdomen with a fistful of sponges to stanch all possible sources of blood loss. Meanwhile, the anesthesiologist administering blood at the head of the table could catch up with the blood loss and hopefully stabilize the patient.
Despite the packs, the soldier continued to bleed from the right upper quadrant, where the bullet had blasted through his liver, shredding the trellis of blood vessels threading both lobes. During the bloodiest moments the surgeons were clamping and tying off large veins that dumped into the dome of the liver under the right diaphragm, finally slowing the torrent. The surgeons packed again, their eyes turning in unison to the monitors at the head of the table to watch as the patient’s blood pressure inched above one hundred and into the normal range.
There were other injuries to contend with too—tears in the stomach, small intestine, and colon that had dumped unsterile gastric contents and stool into the belly, leaving a stew of bacteria, food particles, and freshly clotted blood. The surgeons took a damage-control approach, doing only what they had to do to stop the bleeding, close the holes, and wash out the abdomen. They cut out unsalvageable portions of intestine, stapled across the ends, and covered the abdominal opening with sterile plastic sheets.[12] The soldier’s leg wounds were quickly cleaned, wrapped, and splinted, and he was taken to recovery.
The wounded soldier had received twelve units of fresh whole blood, twelve more units of packed red blood cells, thirteen units of plasma, five units of clotting factors, and a dose of recombinant Factor VIIa, a synthetic clotting drug, and for now he was out of shock and his blood count was near normal. His surgeons had controlled all sources of bleeding and contamination, and everything else that needed to be repaired could wait until he was more stable. Within an hour he would be transferred to a Level III Combat Support Hospital for definitive treatment.
The Forward Surgical Team had made all the right moves and could count this one as a victory. [To see the citations for this excerpt, click here.]
Catherine “Kate” Musemeche, MD is a pediatric surgeon in Austin, Texas. She was previously chief of pediatric surgery and director of pediatric trauma at the University of New Mexico. Visit her blog at www.catherinemusemeche.com.